Latest News
Findings from most recent GLCC Patient Experience Global Survey presented at BTOG24
Findings from the 2023 GLCC global survey of patients’ views on screening for lung cancer and their experience of treatment and care have been presented in a poster at the BTOG (British Thoracic Oncology Group) 2024 conference in Belfast. The poster outlining the survey, its methodology and findings was presented by Jackie Fenemore of Lung […]
Latest issue of UNiTY newsletter out now
The Spring 2024 issue of the GLCC newsletter, UNiTY, is available now. The headline news centres on the publication of our latest international study into awareness of lung cancer symptoms, attitudes towards lung cancer, and views on screening for the disease. All the data from this study is available on the GLCC website HERE. […]
One in three can’t name any symptoms of lung cancer – GLCC study
According to the latest multi-national study published by the Global Lung Cancer Coalition (GLCC), well over one-third of people (37.5%) do not know any symptoms of lung cancer. For young people (aged 18-24) this number is even higher, with 45% of respondents not knowing any symptoms. These numbers are worrying as diagnosing lung cancer […]
New report from Lung Cancer Policy Network – ‘building the evidence base’
From the Lung Cancer Policy Network, 13 February 2024: The Lung Cancer Policy Network has published its 2023 in review: building the evidence base report, detailing what the Network and its members have achieved over the past year. Throughout our outputs and activities in 2023, we sought to demonstrate the breadth of evidence there is to […]
GLCC marks World Cancer Day by publishing data from Global Poll into awareness and attitudes
On World Cancer Day – more must be done to raise awareness Each year World Cancer Day aims to prevent millions of deaths by raising awareness about cancer, and pressing governments and individuals across the world to take action against the disease. Yet, as we mark the 24th anniversary of World Cancer Day, a staggering […]
Fairlife’s 3rd Annual Conference – report
REPORT The 3rd annual FairLife Lung Cancer Care Conference, entitled: “Lung cancer in the spotlight- everyday practice to optimal treatment” concluded successfully FairLife L.C.C.’s activities for November, Lung Cancer Awareness Month. The conference, entitled “Lung cancer in the spotlight – everyday practice to optimal treatment” hosted on Wednesday, November 29, at the ATRAKTOS venue was […]
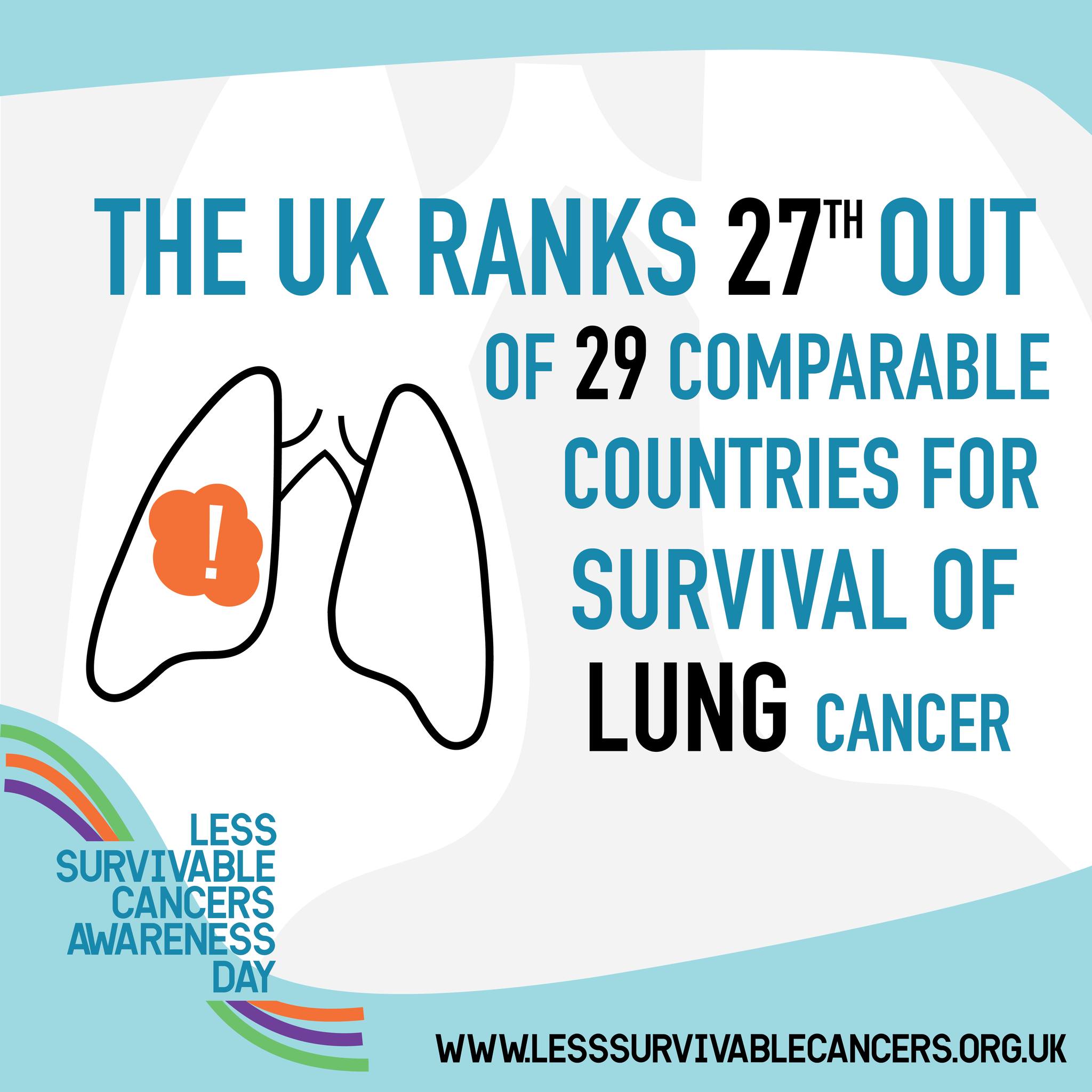
Less Survivable Cancers Day highlights challenges facing UK lung cancer care
UK survival ranks among the worst in the world for deadliest cancers Thursday 11 January 2024 (Less Survivable Cancers Awareness Day) The UK lags woefully behind other countries for cancer survival according to data shared today by the Less Survivable Cancers Taskforce (LSCT). The Taskforce, which represents six less survivable cancers: lung, liver, brain, oesophageal, […]
Lung Cancer Policy Network launches ‘toolbox for change’ report
As members of the @Lung Cancer Policy Network, the GLCC is pleased to have contributed to its latest report: Increasing the earlier detection of lung cancer: a toolbox for change. Earlier detection offers a unique opportunity to shift diagnosis to an earlier stage, and consequently plays a vital role in improving survival by increasing treatment […]
GLCC members’ activities during Lung Cancer Awareness Month
To mark LCAM, here are some images and updates from members across the globe. Throughout the month, we will update this page with messaging and initiatives from our various member organisations, to reflect their LCAM activities. This is by no means an exhaustive list. Please visit the sites or social media channels of our member organisations to […]
Latest edition of our Unity newsletter now available
The new issue highlights the findings of the GLCC’s fourth annual patient experience survey. This year, 712 patients from 14 countries took part, resulting in findings we hope our members, policy makers and campaigners will start to use in their work. Other articles cover: an overview of our Coping With Lung Cancer project FairLife Lung […]
November – Lung Cancer Awareness Month 2023
Lung Cancer Awareness Month – LCAM – observed annually in November, highlights the need for more research to be conducted while cultivating a better understanding of the disease and its challenges. Lung cancer is the leading cause of cancer deaths in men and women worldwide. The disease remains difficult to identify and many individuals don’t […]
Lung Ambition Alliance launches ‘Take The pLUNGe’ LCAM campaign
From our colleagues at Lung Ambition Alliance – November 1, 2023 This Lung Cancer Awareness Month, we’re encouraging you to Take the pLUNGe again! Early detection of lung cancer is key to improving patients’ outcomes and survival.i,ii Lung cancer doesn’t always present outward signs and symptoms, and early detection is critical to ensuring the best […]